Stop worrying, and start living.
I love a good myth-busting sesh, and wanted to bring that here today because it’s been awhile!
You know what I’m talking about. The classic, “joints are wearing out”, it’s the “worst x-ray the doc has ever seen”, and “stretch more to prevent injury”.
We hear this kind of stuff from our clients all the time, sometimes even from other therapists and coaches, and we definitely learned some of it in school.
One of the biggest issues with our professions is that we’re taught to find and obsess over things that are “wrong” because they don’t match a textbook exactly. And then the professionals all work independently; did the knee surgeon talk about rehab and function? Did the doctor explain to you why the imaging results may or may not reflect your pain accurately? Did the therapist show you how the rehab/training plan will actually get you to your goals? Was there consideration of whole body strength training and conditioning?
So no wonder myths start flying, right?
Clients hear them all the time…the scary things about their own concerns, or their loved one’s.
- Bone on bone
- Stretch everything every day
- Disc bulge
- Pinched nerve
- Wear and tear
- Don’t squat
- You’ll break a hip
- Your joint is like an 80 year old’s.
And how many others?
Those phrases are not always accurate though.
They MAY be true statements.
But only for some people, in some situations.
Here’s the thing. Myths get perpetuated reaaaal easy.
And that’s what’s important to note – that some of those things I listed off are myths. Or they’re irrelevant. Or both.
We have newer evidence. We have other approaches and considerations.
So, here’s what we’re gonna hit in this article…
- The real deal about imaging – when it’s used, how it affects rehab, and what it doesn’t actually tell us.
- How wear-and-REPAIR is where it’s at…because wear and tear is old news.
- How to train for injury prevention and mitigation..and sneak peak, it’s not stretching and exercise bands!
By the end of this article, I want you to know – if nothing else – that what is actually accurate, is that
- Scans don’t define the client, their prognosis, or their current function.
- Wear and repair is what actually happens, not wear and tear.
- Injury prevention is more than stretching.
(1) Let’s start with scans, because I know that’s a big one.
I’m talking about X-Rays, MRIs, CTs, everything.
All of them are just pictures. Of some soft tissue or bones, at one moment in time. Now, if you had to choose between looking at a picture or a video of a bike to see what was leading to it not functioning properly, which would you pick? I’d want the video first. The picture could definitely supplement, but I’ll get more info out of the video. And the video in this scan example, is an assessment or screen.
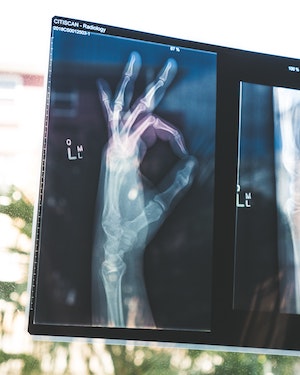
That’s why we need to correlate whatever is on that scan report objectively – look at movement patterns, passively move the joints, test strength, check ligament and cartilage integrity, and everything. Then we can match things up, or rule things out. Those are what matter most when determining a plan. The scan reports play a role – but more often than not, don’t change the rehab or training, at all.
Simply put…Scans are great for ruling out the big bad things – Fractures, tumors, underlying medical conditions.
There are a lot of false positives with imaging – meaning just because it shows a pathology, it does not mean it’s causing or contributing to pain. And that’s because things like disc bulging, cuff tears, and osteoarthritis are a normal part of life. And yes, those things may cause or contribute to symptoms, but the thing i want you to remember, is they also may not. Incidental findings are quite common. That’s why on their own, the things listed on the imaging report aren’t great indicators of prognosis or function.
Here are some specific examples:
- 90% of people between 50-55 years old have age related changes in their spine (but 9/10 people don’t have back pain).
- 48% of people between 20-22 years old have age related changes in a disc, while 25% had a bulge (so there goes that “just getting old” analogy).
- 77% of healthy, pain-free hockey players have hip abnormalities show on imaging.
- 20% of healthy, pain-free adults have partial rotator cuff tears.
These examples are exactly why the person needs to be considered, before the scan. Any why the scan needs to be correlated to the clinical presentation. First, make sure what’s on the scan lines up to the symptoms and what we can measure, and then we can talk about how it might or might not influence prognosis or function.
And if scans have already been done, or are on the docket, that’s totally cool, as it’s all information. And remember that there are always multiple factors contributing – so we can always have some influence, and the scan isn’t the be-all-end-all with decision making.
I want to wrap up this section by saying the opposite can be true too; you can have a lot of pain and a completely normal scan so it doesn’t mean anything is “in your head” or “nothing is wrong”… it just means we ruled out some drivers of pain, as well as all the big bad things, and can move on with conservative training (or psychosocial factors).
(2) “Wear and repair” – this might be my favorite.
I know this might be a big contradiction to what you’ve been told – but hear me out.
We’ve all heard “wear and tear” – and it’s scary AF! Who wants to wear out a bone or joint?! No one! So things escalate to rest, and more stiffness, and more pain.
But really, the opposite is true! The body repairs itself with movement.
Movement at any joint helps move synovial/joint fluid around – which cushions and reduces friction (it’s like WD40) – we want that.
Cartilage lacks it’s own blood supply (it’s nourished through load and compression, when the synovial fluid and all that good stuff gets milked in and around it). In fact, cartilage is produced through load – we know this because astronauts have thinner knee cartilage after coming back from space, and ultra-athletes have thicker cartilage.
I also want to acknowledge that pain has been shown to not necessarily come from the cartilage and osteoarthritis anyways – in 2012 it was noted that 10-34% of patients with a total knee replacement had “bad” outcomes, and 15% of people reported moderate to severe pain 2-5 years after surgery.
To me, that means something else is contributing, not just the cartilage.
Ok. Next. Maybe I lied before, this next (3) “injury prevention is more than stretching section” is actually my favorite…
First off, let’s call it what it actually is – injury mitigation. Because unless you live in bubble wrap and don’t try anything, there’s a chance that injury will happen – because accidents happen. Whether it’s independent like a slip and fall, or related to something like a car accident or sports tackle, we can minimize the damage if we raise the capacity of what you can tolerate.
Sounds great, right?
Great.
Now the specifics you should know…
Stretching and band exercises are not enough for this.
Here’s why.
First, is understanding load and capacity. Injury happens when load exceeds the capacity of a tissue (muscle, bone, anything). So, if load is less than capacity, nothing happens, we’re in that safe zone. If load = capacity, or is slightly more (think positive stress) we are training. However if load quickly or by a lot, overcomes capacity, injury will happen. This is why we talk about strength training being so important throughout the lifetime. It will keep raising, and maintaining the capacity of what your body can tolerate. Both pain, and function.
Next up, is the idea of mobility vs flexibility. They are different. Both good, just in their own ways. Flexibility is what most people typically talk about – they are or aren’t flexible, they need to stretch all the time, etc. And that’s good – sometimes it is important to lengthen a muscle. The key is stretching when it’s actually necessary though, not just because something “feels tight”.
It’s just that mobility is usually what we want – the ability for not only your joint to move through it’s full range of motion, but for you to be able to move it in and out of those positions and to tolerate load in it. Training this is the key. For having the power to get up off the ground. To sit comfortably in whatever position. To minimize injury if you slip and your leg slides out.
This leads well into strength training. Not band exercises. Strength training. Where we may start with bodyweight and bands, and soon progress into using weights, or changing the tempo, or adding holds.
We tend to lose muscle as we age, but it’s more because of less activity and load (or maybe pain and injury) than actual aging. There’s some research out there that shows even if we’re not fully immobilized, we can see measurable muscle loss in a week. Yes, we likely have to work a little harder to get it back in our mature years, but it is possible.
So when we talk about strength training – this means challenge (not struggle). Gradual progressive loading. Law of specificity. Doing what you need to do in real life, in training.
Now, we can talk about the need to train in vulnerable positions. That ankle sprain, arm over the head, bending, reaching, awkward position. If you’ve never gone there in training, tissue quality there will be less-than-ideal, your body doesn’t know how to pull in and out of those positions, or accept load in them (so think back to back to load vs capacity), so injury will happen. Best way to mitigate that injury? Train it before it happens. Gradually expose muscles and joints to various positions and loads, to get them ready with a higher capacity. That’s what’s going to make the difference, and “minimize” injury.
So, to summarize.
- The scan is just a picture. It cannot for sure tell us anything about symptoms, prognosis, or function, unless correlated with the physical presentation in front of us.
- Wear and tear is old news. Science shows us that wear and repair is where it’s at.
- Strength training is key. To help joint health (yay cartilage growth and synovial fluid movement), mitigate damage from injury (shout out higher capacities), and maybe most importantly, allow you the ability to do the things you want and maintain or improve your quality of life.
The choice is yours!
Now stop worrying, and start living ✌🏽
And if you want a sneak peak on how to tell if “feeling” tight truly needs stretching or a different intervention, you can download a quick hamstring screen here, or if you really want to take things to the next level with assessing, rehabbing and training clients with persistent symptoms, check out how we can work together here!
Megan Pomarensky is a Certified Athletic Therapist, a Certified Functional Strength Coach and a Certified Vinyasa Yoga Instructor with a Master’s Degree in Rehabilitation Science.
Over the past 8 years, Megan has built a successful private clinical practice working with clients from professional athletes looking to improve performance to older adults with chronic pain, and everyone in between. Her mission is to empower every client to better understand their body and make informed decisions about their care.
She also helps athletic therapists, trainers and physiotherapists get out of the textbooks, protocols and checklists for better client results.
IG/Twitter @meganpomarensky
www.meganpomarensky.com