Why And How to Program Breathing Exercises
Breathing is a function that is fortunately controlled by our bodies autonomic nervous system. Autonomic control means that our body can effectively regulate respiration without us having to consciously think about every breathe we take. Basically, for the majority of our day our diaphragm and lungs are on cruise control.
The bright side of autonomic control is that not having to remind ourselves 20,000 times a day to inhale and exhale allows for us to focus on other more exciting aspects of life. Unfortunately, lack of consciousness for our breathing patterns can also lead us into trouble.
Somewhere along the way in the everyday shuffle many people will develop postural faults that will lead to inefficient breathing. Compensations in posture and breathing can be triggered in response to emotional stress, injury, poor movement patterning and disease.
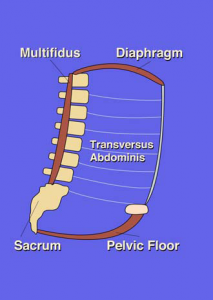
Although frequently going undetected, dysfunctional breathing patterns have the potential to wreck our bodies. Inhibition of respiratory stabilizers like the diaphragm, TVA, multifidus, obliques and the pelvic floor muscles will force your body to rely on other less efficient muscles to keep you alive and breathing. Most often respiratory dysfunction will drive compensatory facilitation upward and downward into the surrounding muscles of the shoulders and hips.
The result is often pain/stiffness in at least 1 of 3 places:
1). Neck/Shoulders (Specifically the Scalenes, SCM and Pectoralis Minor)
2). SI Joint/Lumbar Spine
3). Anterior Hip
Most commonly, I find that Illiacus, Scalenes and Pectoralis Minor are overactive and painful while unnecessarily compensating to assist in respiration.
What’s even worse is that your inefficient breathing has the potential to kick off a chemically driven positive feedback loop, possibly making your already painful dysfunction even worse.
The repeated inefficient gas exchange associated with apical breathing can bring about a shift in pH levels in our bodies. A number of studies have demonstrated that an acidic pH, relative to normal can bring about nasty and painful reactions in the effected soft tissue structures.
Most notably, an acidic pH will stimulate the production of Bradykinin (an inflammatory pre-cursor), increase pain threshold sensitivity and promote the development of taut bands resulting in trigger points.[i] This cascade pushes our body further into a state of stress, continuing the painful cycle.
In order re-program our respiratory muscles and develop efficient core function we must practice our breathing pattern just like we would any other pattern. Reconditioning the muscles of our pelvic canister (diaphragm, transverse abdominis, pelvic floor, obliques and multifidi) not only proves valuable in treating dysfunction and improving movement quality but can also serve as a window into our parasympathtic nervous system. By practicing controlled breathing we have the ability to shift our bodies into a parasympathtic state. All of this is good news as it relates to optimizing our internal environment for rest and recovery.
There are a number of ways you can incorporate breathing into your therapy and training programs. I have found them extremely valuable in my therapy practice assisting in joint re-positoning and equally as useful on the gym floor in improving my mobility drills. Check out below to see how I prefer to implement breathing exercises into my training programs.
Teaching Drills
Prone Breathing
This prone breathing drill is a great place to start with new clients who are initially re-learning a basic breathing pattern.
Lie face down on the ground with your hands supporting your forehead. Focus on breathing in deeply through your nose and out through your mouth. You should be actively trying to inhale air into your abdomen and expand laterally through your midsection with each breath. Actively try to breath out on each exhalation, by contracting your abdomen. Perform for 1-2 minutes.
90/90 PRI Breathing with Balloon or Straw
The 90/90 position breathing drill is an exercise I learned while taking the PRI Myokinematic Restoration course. I have found this drill to be extremely effective at re-establishing the zone of apposition in clients who are chronically overextended. This is frequently my first choice when treating clients with shoulder mobility and and hip impingement issues.
Lie on your back with your hips and knees flexed to 90 degrees and your heels placed on the seat of a chair or box. Breathe in deeply through your nose while focusing on expanding your abdomen and rib cage laterally. Breathe out forcefully through your mouth, focusing on depressing your ribs inferiorly and expelling all of the air in your lungs. Following the end of the first exhalation slightly posteriorly tilt your pelvis by driving your heels into the chair, lifting your butt about 2 inches off the ground. Hold the posterior tilted position for the remainder of the exercise and complete 4 more breathe cycles. Following the 4th breathe relax, drop your hips and repeat the drill 1-2 more times.
Breathing With Stretching And Movement
I especially find breathing effective when incorporated into my stretching and mobility drills. Facilitating a series of quality breathes into your movement drills will significantly increase their effectiveness. Additionally, I have begun prescribing all of my stretching drills by breath counts rather than time. So, instead of having a client stretch for 30 seconds I will ask that they hold the position for “10 good breathes.” I have found that this technique not only enhances the stretch itself but demands that the client is much more mentally engaged in the drill. Check out some of my favorite drills shown below.
Active Box Hip Flexor with Breathing
Lateral Squat with Breathing
Wallslide with Breathing
T-Spine Mobilization with Breathing
Recommended Related Articles
The Value Of Blowing Up A Balloon
Interview with Leon Chaitow, Stress, Breath, Fascia and pH
By Kevin Carr, C.S.C.S., LMT
Contact: Kevin@Movement-As-Medicine.Com
[i] Shah, J., and E. Gilliams. “Uncovering the Biochemical Milieu of Myofascial Trigger Points Using in Vivo Microdialysis: An Application of Muscle Pain Concepts to Myofascial Pain Syndrome.” Journal of Bodywork and Movement Therapies 12.4 (2008): 371-84. Web.